Translate this page into:
Giant epigastric hernia induced by the second stage of labor in an obese multigravida: A case report

*Corresponding author: Ubong Bassey Akpan, Consultant, Department of Obstetrics and Gynaecology, University of Calabar Teaching Hospital, Calabar, Cross River, Nigeria. ubongabasiakpan@gmail.com
-
Received: ,
Accepted: ,
How to cite this article: Akpan U, Nwagbara V, Asibong U, Okpeberi K. Giant epigastric hernia induced by the second stage of labor in an obese multigravida: A case report. Calabar J Health Sci 2020;4(1):44-7.
Abstract
Several acute undesired events can occur during the second stage of labor due to a significant increase in the intra-abdominal pressure associated with the process of expulsion of the fetus. Herniation of loops of the bowel due to sudden separation or tear in the rectus fascia in a woman without the previous abdominal surgery is a very rare occurrence. We report a case of intrapartum herniation of intra-peritoneal viscus through a large epigastric defect that occurred during the second stage of labor.
Keywords
Labor
Anterior abdominal wall
Hernia
INTRODUCTION
Abdominal wall hernias are common, especially at the inguinal canal and periumbilical area due to the natural anatomical weakness or the defects in the fascial surrounding these points.[1] However, giant epigastric hernias are rare.[2] A hernia is said to occur more frequently among young males than women, and surgical procedures for hernia are among the most common operative procedures in young African males.[2]
The risk factors for abdominal wall hernia are numerous. Family history and strenuous occupation are the most documented risk factors in Nigeria.[2] Pregnancy and obesity are, however rare risk factors.[3,4] The prevalence may also vary with cultures. A study in Saudi Arabia has reported more prevalence among women and pregnancy, obesity, and constipation were major risk factors.[5] In that study, the most frequent site of occurrence was the inguinal region. A study in India reported that hernia repair procedures accounted for 15–18% of all surgical procedures in that country, and males were at greater risk due to biological variability.[6]
Repeated pregnancy and process of childbirth, especially vaginal delivery, may induce sub- clinical or insidious abdominal wall hernias, but sudden protrusion of giant hernia due to the separation of the rectus fascia during labor is a very occurrence. In a search of the literature, only one case of intrapartum rupture of umbilical hernia has been reported. We report a rare case of huge epigastric hernia induced by intra-peritoneal pressure during the second stage of labor.
The second stage of labor refers to the stage from the full cervical dilatation to the complete expulsion of the fetus through the vagina. The woman/patient is usually encouraged to perform valsava maneuver during uterine contraction and bear down with contraction. This increases in the intra-abdominal pressure exert a force on the uterus and its content, which facilitates the delivery of the baby. This excess intra-peritoneal pressure may be detrimental to some women.
CASE PRESENTATION
The patient was a 33-year-old G6P3 (three alive) women who received her antenatal care in the University of Calabar Teaching Hospital. She was a businesswoman by profession. She has had two previous spontaneous vaginal deliveries of babies of average birth weights in the same hospital in 2013 and 2014. The delivery of the first two babies was not complicated. She had not noticed any significant abdominal swelling or been diagnosed of hernia before pregnancy and delivery. The third pregnancy was also registered at the same tertiary hospital. The antenatal period was uneventful. She promptly presented to the labor ward in the early onset of labor. The first stage of labor was not prolonged and not precipitated. When the cervix was fully dilated (second stage of labor), she was transferred to the delivery couch, where she was encouraged to bear down with uterine contraction. About 15 min into the second stage of labor while bearing down for the delivery of the baby, she experiences a sudden tearing pain in the epigastrium that was accompanied with a large protrusion of a giant hernia in the epigastric area. Following the delivery of the baby, the hernia was reducible and the pain subsided. The puerperium was uneventful. She was counseled for the repair of the hernia. However, the patient opted for the procedure to be performed in her subsequent delivery, where she has also indicated her interest in cesarean section as the option for the subsequent delivery.
She conceived again in 2018 (last menstrual period, October 24, 2018). The pregnancy was uneventful during the antenatal period. She was reviewed by a general surgeon in preparation for cesarean – herniorrhaphy and abdominoplasty.
She was admitted to the antenatal ward at a gestational age of 38 weeks in preparation for cesarean delivery. On physical examination, she was an obese young woman, her height was 1.67 m, and her weight was 122 kg, giving the body mass index of 43.7 kg/m2 (at pre-pregnant).
The examination of the abdomen revealed a gravidly enlarged abdomen. There was a bulge of hernia about 5 cm from the xiphisternum along the midline with a round shape in the anterior abdominal wall [Figure 1]. There was visible intestinal peristalsis within the protrusion. The mass measures 20 cm in its widest diameter. It was reducible with minimal tenderness.
Ultrasound scan done revealed a massive defect in the anterior abdominal wall with herniation of gut into the sac.
The cesarean section and the abdominal hernia repair were performed on November 30, 2019, at the gestational age of 38 completed weeks.
Epidural (regional) anesthesia was used. The baby was delivered through a low transverse (Pfannenstiel) incision. The baby was a live male infant weighing 3.5 kg with good Apgar scores. The herniorrhaphy and the abdominoplasty were performed by the general surgeon following closure of the Pfannenstiel incision.
Hernia repair
The skin over the epigastric swelling was excised. The margin was defined (about 20 cm in its widest diameter), as shown in Figures 2 and 3. The hernia sac had loops of bowel and part of the omentum. The bowel was examined for viability and peristalsis was demonstrated. There was no evidence of gangrene. There were mild intra-peritoneal adhesions between the omentum and the mesentery of the transverse colon. The adhesions were separated. The redundant sac and the surrounding skin were excised. Mass closure of the defect was done with nylon two monofilament non-absorbable suture in continuous fashion. The skin was then closed with polyglactin suture 2/0 subcuticular stitches. Sterile wound dressing was applied. She was given broad-spectrum antibiotics and analgesics.

- Giant epigastric hernia during pregnancy.

- Surgical repair of the hernia.
Her post-operative period was uneventful except for subdermal edema which was managed conservatively. She was discharged home on the 8th post-operative day.
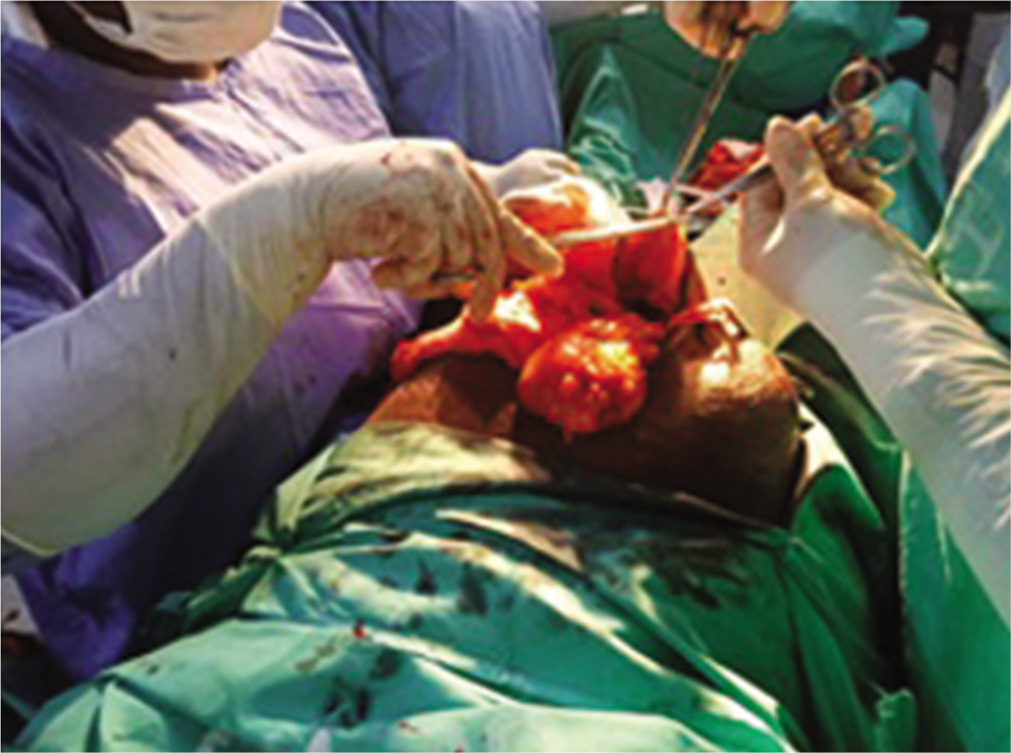
- Large hernia sack with its contents.
DISCUSSION
Intrapartum abdominal wall herniation during the second stage of labor is a very rare occurrence, especially where there was no previous defect in the rectus sheet or previous abdominal surgery. Most cases of hernia usually present insidiously and gradually enlarge over period of months or years.
Emergency surgical procedures are often indicated when there is obstruction or strangulation of the hernia contents at the neck of the hernia sac.[3,7]
Another indication for emergency repair is when there is a rupture of hernia sac due to blunt or penetrating trauma.[8] Delayed or interval repair of the defect is often chosen if there is no immediate risk to the patient.[2,8] On the index patient, there were no signs or symptoms of strangulation. The hernia content was reducible. After a thorough evaluation following its occurrence in the intrapartum period, the options of treatment were discussed with the women. She opted for cesarean herniorrhaphy in her subsequent pregnancy. This saves the cost of treatment and minimizes the risk of repeated exposure to anesthetic agents. It also allows the woman and her family members to make adequate preparation for the surgical procedure and choice of contraception.
Interval repair of a hernia during cesarean section can also be chosen in cases of incisional hernias occurring following previous abdominal wall surgeries.[9]
The choice of incision is also important as many women will prefer a single surgical scar instead of multiple scars for aesthetic reason. In cases of incisional hernia following a previous cesarean section scar, it is proper to enter the abdominal cavity for the repeat cesarean section through the previous scar. The repair of the hernia is done after closing the uterine incision.[9] In the index patient, the site of occurrence was far from the lower uterine segment as such a single extended midline incision was not desirable.
Surgical repair of hernia may be done using laparoscopic technique or open repair.[7] In the index patient, we used open abdominal surgery approach due to the pregnancy state and the size of the defect. A laparoscopic approach may be preferred in a non-pregnant patient with a small hernia.[7,10]
The surgical technique used for abdominal wall closure is believed to significantly influence the risk of recurrence.[7,10] In a recent systematic review, open surgery and laparoscopic surgery for the repair of hernia have a similar rate of recurrence (odds ratio 0.419, 95% confidence interval 0.159– 1.100; P = 0.077).[10]
Repair of hernia is associated with significant improvement in the quality of life in the individual patient, as evidenced in the index patience who admitted that the occasional abdominal discomfort, she was experiencing disappeared following the successful repair of the hernia. Another study that focused on the quality of life reported significant improvement in patient quality of life a year after repair of a hernia (P < 0.001) in relation to fatigue, domestic activity, and pain.[11]
Reconstruction of giant midline abdominal wall fascia defect or rectus sheet may be approached in several ways. Large fascia defect can pose a surgical challenge to the surgeon during primary closure. The use of prosthetic material and mesh has been advocated, but is not without complication. The commonly reported complications include allergy, wound infection, enterocutaneous fistula, and chronic irritation.[12] This is usually indicated if there is no sufficient tissue to close the defect.
In such cases, prosthetic materials may be used. This is considered to be the most frequent method of reconstruction of a large ventral hernia.[12] However, the risk of infection may be catastrophic, especially if there is post-surgical wound infection.[11] Pregnancy is associated with low body immunity due to decreased B-cells activity and the high serum levels of endogenous steroids produced in the placenta.[13] Another problem to be considered is that of an allergic reaction to the substance of the mesh. In the index patient, the fascia gap was easily apposed and aligned properly following the delivery of the baby; then, continuous monofilament non-absorbance suturing was done to maintain the integrity of the fascia. This method reduces the recurrence rate and minimizes the risk of infection associated with the use of mesh. In one study, 40% of the patient with giant hernia have to remove the mesh due to infection.[12]
CONCLUSION
Giant epigastric hernia occurring during the second stage of labor is a very rare complication and can be distressing to the patient. The decision to embark on immediate repair or delayed repair depends on the clinical presentation, risk of incarceration, or obstruction as well as patient’s choice. The obstetrician may often seek the expertise of a general surgeon for a good outcome.
Declaration of patient consent
Patient’s consent not required as patients identity is not disclosed or compromised.
Financial support and sponsorship
Nil.
Conflicts of interest
There are no conflicts of interest.
References
- Abdominal wall hernias: Imaging features, complications, and diagnostic pitfalls at multi-detector row CT. Radiographics. 2005;25:1501-20.
- [CrossRef] [PubMed] [Google Scholar]
- Hernia in South Southern Nigeria: Five year retrospective study. IOSR J Dent Med Sci. 2016;15:96-111.
- [CrossRef] [Google Scholar]
- Frequency of abdominal wall hernias: Is classical teaching out of date? JRSM Short Rep. 2011;2:5.
- [CrossRef] [PubMed] [Google Scholar]
- Risk factors for inguinal hernia in adult male Nigerians: A case control study. Int J Surg. 2012;10:364-7.
- [CrossRef] [PubMed] [Google Scholar]
- Prevalence, risk factors and characters of abdominal hernia in Arar City, Northern Saudi Arabia in 2017. Electron Physician. 2017;9:4806-11.
- [CrossRef] [PubMed] [Google Scholar]
- Incidence of inguinal hernia and its type in a study in a semi-urban area in Andhra Pradesh, India. Int Surg J. 2016;3:1946-9.
- [CrossRef] [Google Scholar]
- Laparoscopic vs. Open incisional hernia repair: A randomized clinical trial. JAMA Surg. 2013;148:259-63.
- [CrossRef] [PubMed] [Google Scholar]
- Traumatic anterior abdominal wall hernia: A report of three rare cases. J Emerg Trauma Shock. 2011;4:142-6.
- [CrossRef] [PubMed] [Google Scholar]
- Short term outcomes for open and laparoscopic midline incisional hernia repair: A randomized multicenter controlled trial: The ProLOVE (prospective randomized trial on open versus laparoscopic operation of ventral eventrations) trial. Ann Surg. 2013;238:37-45.
- [CrossRef] [PubMed] [Google Scholar]
- The treatment of incisional hernia. Dtsch Arztebl Int. 2018;115:31-7.
- [CrossRef] [PubMed] [Google Scholar]
- Staged management of giant abdominal wall defects: Acute and long-term results. Am Surg. 2003;238:349-55.
- [CrossRef] [PubMed] [Google Scholar]
- Repair of giant midline abdominal wall hernias: Components separation technique versus prosthetic repair: Interim analysis of a randomized controlled trial. World J Surg. 2007;31:756-63.
- [CrossRef] [PubMed] [Google Scholar]
- The immune system in pregnancy: A unique complexity. Am J Reprod Immunol. 2010;63:425-33.
- [CrossRef] [PubMed] [Google Scholar]






