Translate this page into:
Assessment of the knowledge of radiology in exiting medical students in University of Calabar

*Corresponding author: Samuel Archibong Efanga, Department of Radiology, University of Calabar, Calabar, Cross River State, Nigeria. samuelefanga@rocketmail.com
-
Received: ,
Accepted: ,
How to cite this article: Inah GB, Efanga SA. Assessment of the knowledge of radiology in exiting medical students in University of Calabar. Calabar J Health Sci 2021;5:45-52.
Abstract
Objectives:
Radiology education in the undergraduate level imparts in medical students the basic knowledge to interpret common pathological conditions, know the right imaging requests to make and the right order in which they should be made when they become physicians and the degree of this knowledge is influenced by several factors. The aim of this study was to evaluate the knowledge of radiology in exiting medical students and to identify the challenges of undergraduate radiology education.
Material and Methods:
This was a prospective cross-sectional observational study that was conducted in a 2-month period in the Radiology Department of the University of Calabar Teaching Hospital. The year 6 medical students of the University of Calabar, who were 79 in number, participated in the study. Relevant questions covering the major areas of radiology were presented to each participant by the use of a pre-test questionnaire. SPSS version 23.0., Pearson’s Chi-square test, and t-tests were used to analyze the data.
Results:
The medical students had a mean score of 66.5% in radiology knowledge. A significant relationship was observed between diagnostic radiology knowledge and the duration of radiology posting (P = 0.029), radiology teaching methods (P = 0.001), and the quality of learning environment (P = 0.002), respectively.
Conclusion:
The final year medical students in University of Calabar have an appreciable knowledge of radiology. This can be improved if the duration of radiology education increases by early introduction into the pre-clinical class or other clinical courses, if the radiology teaching methods are updated, and if the quality of the learning environment is improved.
Keywords
Medical students
Radiology
Education
Knowledge
INTRODUCTION
Radiology is an invaluable component in clinical medicine, central in the diagnostic process, as well as offering therapeutic options for patients. For almost 100 years, the format of teaching medical students radiology has evolved from tutorials by the early Professors of Radiology (1925–1950), through the calls for compulsory radiology lectures for medical students when it later became an elective course and ultimately in the 1980s, it was made a compulsory clerkship for medical students.[1]
It is disappointing that despite the indispensable role, radiology plays in modern-day medicine, it has yet to be proportionally reflected in the training curriculum in medical schools and in the quality of knowledge expressed by the undergraduates.[2] Surveys indicate that medical students are poorly prepared for medical practice with regard to the interpretation of radiological images and clinical leaders have impressed on the university policy-makers the need for an increase in the radiological input into medical student education.[1-3] Failure to intervene in this trend may lead to a high rate of patient management errors and adverse outcomes.[4]
Physicians are prone to underestimating the actual doses involved in requested radiological procedures and have poor knowledge of the possible risks that these tests portend to the health of the population.[5,6] Surprisingly, the number of referrals for pediatric CT studies has skyrocketed, increasing concerns regarding cancer risks in this highly radiosensitive population.[7]
There is growing interest in exploring complementary radiological instructional approaches that would efficiently fill in existing knowledge gaps, foster application of knowledge stores, promote higher order thinking, and better prepare students for the challenges of clinical decision-making.[8]
The aim of this research was to assess the knowledge of radiology in the 6th year medical students with respect to clinical practice and to identify the challenges of undergraduate radiology education with a view to recommend ways of improving it.
MATERIAL AND METHODS
This was a prospective cross-sectional observational study conducted from April 2021 to May 2021 at the Radiology Department of the University of Calabar Teaching Hospital, Calabar, Cross River State, Nigeria. Ethical approval was obtained from the Health Research Ethics Committee of the University of Calabar Teaching Hospital.
The study population comprised 6th (final) year medical students of the University of Calabar (UNICAL), Calabar. A questionnaire, which utilized the Likert scale response system and the Yes or No response pattern, containing 50 items, was administered to the surveyed participants. The questions in the questionnaire were brief and easy to understand.
The final year medical students were invited to the radiology department where an in-depth explanation of the objectives of this research was done. The consent forms were passed to the willing participants and those who met the inclusion criteria. All 79 members of the 6th year class gave their consent. The participants were informed to revise the lecture notes obtained during their radiology posting in preparation for the exercise. A 1-month period was provided for the revision process.
The consented students presented themselves 1 month later for the administration of the questionnaire. They were divided into two groups to ensure adequate spacing and that each participant’s thought or response was not influenced by another. The duration allotted for the exercise of filling the questionnaire was 1 h.
The questionnaire was designed by clinical radiologists who also lecture medical students. The questionnaire was divided into several sections for all the participants to tick using Yes or No (in sections B, C, D, and E) and the Likert scale (in sections A, F, and G);
Section A
This segment assessed their general opinion on clinical radiology posting and the conduciveness of the radiology learning environment.
Section B
This segment assessed the knowledge of the medical students on the most appropriate image modality to be selected for different clinical scenarios.
Section C
This segment assessed the knowledge of the risk of ionizing radiation and how to protect a patient from its unnecessary exposure.
Section D
This segment evaluated the adequacy of clerkship in the radiology training of medical students.
Section E
This segment assessed the ability to recognize or interpret lesions in radiological images and to appreciate and corroborate these features when radiologists write reports based on their diagnostic knowledge of radiology.
Section F
This segment assessed the opinions of medical students on the necessity of introducing radiology education in the pre-clinical classes.
Section G
This segment acted as a feedback on the opinion of the efficacy of the present radiology teaching methods, potential modifications, and the possible ancillary teaching avenues.
The data obtained were analyzed using the Statistical Package for the Social Sciences (SPSS) for Windows (SPSS Inc., USA) version 23. Appropriate descriptive (including simple proportions and percentages) and inferential statistical methods were used to analyze the data and tables, bar charts and pie charts were the means of displaying the result where applicable. Continuous variables were reported as means and standard deviation (mean ± SD). Pearson Chi-square test of independence was used to analyze individual questions and determine the presence of relationships. Statistical significance was defined at P < 0.05.
RESULTS
Seventy-nine (79) medical students were recruited into the study; this consisted of 48 (60.8%) males and 31 (39.2%) females. The age and sex distribution of the subjects are shown in Figure 1. The majority of them (84.8%) were in the 20 to 29 years age group.
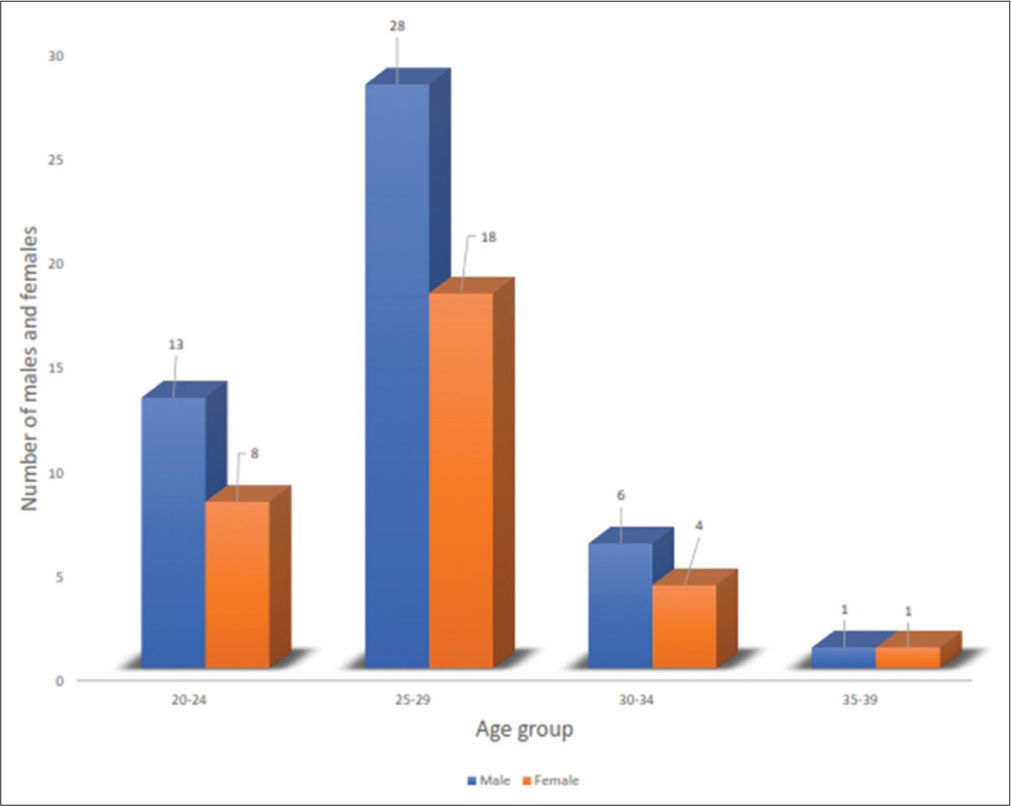
- Distribution of males and females within the age groups.
The number of female medical students who have correct knowledge lagged behind that of the males in all three sections meant to assess their knowledge in Radiology and this is shown in Figure 2. The ratio of the males to the females who had correct knowledge in the three sections were as follows; 3:2 in the image selection knowledge section, 7.8:5 in the Radiology risk knowledge section and 3:2 in the diagnostic Radiology knowledge.

- Determination of the level of correct knowledge in the male and female medical students on appropriate image selection knowledge, radiation risks knowledge and diagnostic radiology knowledge.
The responses that showed correct knowledge and incorrect knowledge in the three major sections used to assess the knowledge of Radiology in medical students is displayed in Figure 3. Across the three sections an average score of 66.5% was recorded.

- The scores obtained by the medical students on appropriate image selection knowledge, radiation risks knowledge and diagnostic Radiology knowledge.
Table 1 shows the opinion of the students on the duration of Radiology posting, Radiology teaching methods and the quality of the learning environment. These were noticed to have significant effect on the scores obtained during the assessment of their level of knowledge in Radiology during this study with P values of 0.029, 0.001 and 0.002 respectively.
| Diagnostic radiology knowledge | |
|---|---|
| P value | |
| Duration of radiology posting | 0.029 |
| Radiology teaching method | 0.001 |
| Quality of learning environment | 0.002 |
P<0.05 is statistically significant
Table 2 shows the distribution of the students’ opinions on the present quality and training modalities utilized in Radiology education. A large number of the medical students (93.7%, which is the sum of those who agreed and strongly agreed) were in support of interactive sessions during Radiology lectures. The flipped classroom method, which employs e-learning resources, was preferred by 88.6% of the medical students (who agreed and strongly agreed), as an ideal mode of teaching Radiology. Also, 67.1% of the students strongly agreed and agreed that the duration of Radiology was not adequate.
| Strongly agreed and agreed |
Neutral | Strongly disagreed and disagreed |
P value |
|
|---|---|---|---|---|
| The duration of posting in radiology is adequate | 14 | 12 | 53 | 0.187 |
| The lecturers spent adequate time with us | 24 | 19 | 36 | 0.035* |
| The environment was cool and comfortable | 43 | 16 | 20 | 0.089 |
| Is it ideal to teach radiology as a course in the pre-clinical classes? | 48 | 9 | 22 | 0.148 |
| Is it ideal to merge radiology with anatomy lectures? | 55 | 12 | 12 | 0.208 |
| It will be better if radiologists partake in the radiology explanation of normal anatomy? | 64 | 12 | 3 | 0.300 |
| The radiology teaching method that involves sending images/ or + employing E-learning resources and teaching notes to you before the lecture is ideal? | 70 | 6 | 3 | 0.351 |
| During lectures in radiology, is a student- teacher interactive session ideal and should be adopted? | 74 | 4 | 1 | 0.385 |
P<0.05 is statistically significant
Table 3 shows the number of the students who were knowledgeable of the type of radiation produced by Ultrasound scan (US), Computerized Tomography (CT) scan and Magnetic resonance Imaging (MRI) scan. Those with the correct knowledge of the fact that both MRI and US make use of non-ionizing radiation accounted for 84.8% of the medical students recruited for the study and this consisted of 61.2% males and 38.8% females. Also, 62% of the students (which consisted of 61.2% males and 38.8% females) know that CT is not safe for neonates while 89.9% of the entire students (which consisted of 62% males and 38% females) were aware that CT scan is not safe for fetuses.
| Correct knowledge | Incorrect knowledge | P value | |||
|---|---|---|---|---|---|
| Male | Female | Total | Total | ||
| MRI and US make use of ionizing radiation | 41 | 26 | 67 | 12 | 0.387 |
| In a 1-month-old child with suspected hydrocephalus, a CT scan is ideal? | 30 | 19 | 49 | 30 | 0.150 |
| It is ideal for a 10 weeks pregnant woman to be sent for a pelvic CT scan? | 44 | 27 | 71 | 8 | 0.035* |
P<0.05 is statistically significant
Table 4 shows the degree of adequacy of clerkship among the subjects during Radiology posting. Very few of the medical student (6.3%) observed at least 5 CT scan procedures and just 7.6% observed special procedures in the Radiology department. Only 36.7% of the students observed the reporting of at least ten (10) conventional radiographs.
| Yes | No | Total | P value | |
|---|---|---|---|---|
| In your radiology posting did you observe at least five ultrasound procedures? | 49 | 30 | 79 | 0.150 |
| In your radiology posting did you observe at least five CT scan procedures? | 5 | 74 | 79 | 0.457 |
| In your radiology posting did you observe the reporting of at least 10 films (radiographs)? | 29 | 50 | 79 | 0.165 |
| In your radiology posting did you observe any of a barium swallow, barium meal, or an IVU procedure? | 6 | 73 | 79 | 0.448 |
P<0.05 is statistically significant
DISCUSSION
The Medical College of the University of Calabar (UNICAL) has Radiology education within its academic curriculum, which is spread over a two-week period that encompasses 42 - 45 hours of teaching. In the United Kingdom the time dedicated for the teaching of Radiology to medical students is between 44 – 116 hours and variations in lecture duration is noted in other countries; New Zealand – 276 hours, USA – 165 hours, Australia – 85 hours, Pakistan – 40 hours. The difference in the time range reported for different countries is attributed to the inclination of the University Chairs in Radiology (the most senior Radiologist or Radiology head of Department) towards the adequacy of Radiology education.[1,6] The total hours spent on Radiology education of medical students in UNICAL seems to be relatively meager.
A large number of students in this study shared similar concerns with 67.1% strongly disagreeing or disagreeing that the duration of posting in Radiology was adequate. Majority of the students (53.2%) in Salaam et al’s[6] study also opined that the time given for Radiology lectures was not adequate. This was corroborated by an Indian based study conducted by Vinod et al.[9] who reported that 52% of the students felt that the period for Radiology posting was not adequate. The medical students in UNICAL further expressed dissatisfaction with the time that the Radiology lecturers spent with them as 45.6% strongly disagreed or disagreed on its adequacy while 30.4% (who strongly agreed or agreed) felt that it was adequate.
One of the viable measures than can be adopted to increase the time set aside for Radiology education in UNICAL is its introduction into the pre-clinical class schedule. Bhogal et al.[2] also favours an early introduction of Radiology into the training scheme for medical students by the University policy makers. They are inclined to the view that exposure to Radiology training at the pre-clinical stage brings about a deeper understanding of the basic sciences while in the clinical stage medical students will get to understand how intrinsic Radiology is to the diagnostic and management decisions of patients.[2] More than half (60.8%) of the students in this study strongly agree and agree that it is ideal to include Radiology as a course in the pre-clinical classes.
Many countries in Europe introduce Radiology into the curriculum for medical students in the 1st year of their program. However, in Greece it commences at the 4th year while in Italy it is introduced in the 5th year. The United Arabs Emirate university, in Asia, has it incorporated into the 6th year academic program. In the UK 85% of medical schools offer Radiology training in more than 1 academic year and about a quarter of these institutions provide the training every year.[2] In the Medical College of the University of Calabar, Radiology education is presented to the medical students in the 5th year.
The medical students in UNICAL feel that it is ideal to merge Radiology with Anatomy in the pre-clinical classes as 69.6% strongly agreed or agreed with the idea while 15.2% either strongly disagreed or disagreed. Jack et al[10] noted that 90% of medical schools who had merged Radiology education into the anatomy curriculum had at least one member of the Radiology department. About 50% of the surveyed institutions have a Radiology fellow as a faculty member of the anatomy department, which allows a continuous anatomy learning that bridges the gap between clinical medical practice and basic medical sciences.[10]
About 58% of chairs and 53% of deans inferred that more Radiologists were needed to be involved in medical imaging education.[3] It has been suggested, as an action plan, that there should be an aggressive promotion of Radiologists as integral to every anatomy course, to become the face of imaging at the beginning of the students’ educational experience.[3] There was an overwhelming congruity with these suggestions by the students in this study as 81% strongly agreed or agreed that it will be ideal if Radiologists were involved in the explanation of the Radiology of normal anatomy while 3.8% strongly disagreed or disagreed.
In this study we found out that the students’ knowledge of the imaging modalities that employ ionizing radiation and that of the organs that are highly sensitive to this radiation was encouraging as 84.8% had correct knowledge. However, 15.2% had incorrect knowledge of the fact that Ultrasound scan (US) and Magnetic resonance imaging (MRI) did not make use of ionizing radiation. Dellie et al.[5] found out that 71.4% and 79.3% correctly believed that US and MRI, respectively, employed non-ionizing radiation in its function as a radiological tool for diagnostic purpose. Murphy et al.[11] reported that 81% and 50% of medical students correctly identified that US and MRI, respectively, did not lead to ioniz.
Murphy et al[11] reported that 81% and 50% of medical students correctly identified that US and MRI, respectively, did not lead to ionizing radiation exposure. The findings in the diverse studies from different climes are very similar and of a good knowledge level.
In the present study, 89.9% and 62% of the medical students had correct knowledge that fetuses and neonates respectively, were more sensitive to the effects of ionizing radiation. O’Sullivan et al[7] observed that 80% of their study population had correct knowledge of the high sensitivity of children to ionizing radiation than adolescents.
Correct knowledge of the type of radiation emitted by MRI and US was noted in approximately 62% of males and 38% of females in our study. O’Sullivan et al[7] noticed that more females than males thought that MRI made use of x-rays (20% compared to 11%, P 0.009), which was in line with the widely found scenario that males appeared to be more knowledgeable in Radiology.
In terms of the overall knowledge of radiation risks, 80% of the UNICAL medical students had correct knowledge (60.9% of them were males and 39.1% were females) while 20% had incorrect knowledge. Bhogal et al[2] noted a below par performance where it was reported that only 47% of the undergraduates in a study had correct knowledge of radiation risks assessments.[2]
This study assessed the image selection knowledge in the undergraduates and observed that 56.5% (consisting of 60% males and 40% females) had good knowledge while 43.5% had incorrect knowledge. An identical situation was seen in a New Zealand based study as it was noted that the respondents achieved a mean score of 53% for selecting the appropriate imaging modality to be requested for in certain clinical scenarios.[2] This is not a good development and does not augur well for the immediate future of clinical medicine. The proportion of undergraduates with incorrect knowledge of image selection in this study (43.5%) was high and may lead to an increase in the number of wrong radiological requests made for patients who are probably in deplorable financial states. This causes delay in making the right clinical management decisions with potentially devastating outcomes on the patient.
Medical students are expected to acquire knowledge of certain pathognomonic radiological features of common pathologies for clinical comprehension of radiological reports and the accompanying images during their clinical practice. It was depicted in this study that 63% (which comprised of 60% males and 40% females) of the medical students in UNICAL had correct knowledge of diagnostic radiology while 37% had incorrect knowledge. Salaam et al,[6] in a study in Jos, Nigeria, observed that 60 (49.6%) of the undergraduate students had correct knowledge of diagnostic radiology while 61 (50.4%) of the undergraduate medical students had incorrect knowledge of diagnostic radiology. This demonstrated that the students in their study had a below average knowledge of diagnostic radiology which was not a good outcome.[6] In this study it was seen that the opinion of the UNICAL medical students on the duration of Radiology posting had an impact on the scores obtained during the assessment of their knowledge of diagnostic radiology (P 0.029) which could be the bane of the poor performance of the undergraduate medical students in Saleem et al’s[6] research. On the contrary, it was encouraging to note that Vinod et al[9] found out that 71 (59.2%) students had correct knowledge of diagnostic Radiology while 49 (40.8%) students had incorrect knowledge of diagnostic Radiology.
In a Palestinian based study, Awadghanem et al[12] noted that male participants achieved a higher score in general radiology knowledge assessment when compared to female participants (P 0.034). This is consistent with the results of our study. Probably male students were encouraged to pursue a career in Radiology than their female counterparts were and this encouragement likely heightened the interest of males to learn more during the posting.[12] Vinod et al[9] observed that male undergraduate students who showed fondness for Radiology were 75 in number compared to 25 female students. They had the notion that this was probably because there were more male entrants into most medical schools than females. Their observation was corroborated by this study which showed that there were more undergraduate males than females in the class involved in the research.
It is evident that there is some degree of displeasure and discontent with the avenues that have been utilized to teach Radiology. About 47.6% of students in Salaam et al’s[6] study concurred that Radiology teaching mode was inadequate for an effective education. This view was seen in other studies where it was noted that few students, 19% and 42%, respectively, felt that they had received sufficient Radiology education and the teaching mode was adequate.
This view was seen in other studies where it was noted that few students, 19% and 42%, respectively, felt that they had received sufficient Radiology education and the teaching mode was adequate.[2,9] In our study it was shown that the students’ opinion on Radiology teaching mode had significant impact on their scores on the knowledge of diagnostic Radiology (P 0.001), this implies that the pattern of Teaching Radiology has to be re-evaluated.
Flipped classroom pedagogical approach encourages medical students to independently learn basic facts and concepts outside the classroom through reading, completing online educational modules and watching a variety of several E-learning resources (including Instagram). In the classroom afterwards, the Radiology educator will engage the medical students in a more interactive case-based or system-based sessions which are geared towards the generation of radiological skills and their application in a clinical setting. Moreover, it affords the instructor the opportunity to identify the concepts and skills that proved challenging to individual medical students and attempt to effect illumination and consequently, promote mastery.[8,13-16]
Salajegeh et al[4] found out in their study that a majority of the undergraduate medical students (71.4%) felt that the E-learning package was effective in helping them learn the art of interpreting X-rays. Sait et al[14] realized that the medical students in their study were in support of this opinion when 100% of the participants agreed or strongly agreed that E-learning in Radiology was appropriate and should be recommended to other colleagues. Nyhsen et al[15] thought otherwise by stating that E-learning module was relatively poorly rated and should be regarded as a less effective method of learning.
It was observed in this study that 88.6% of the medical students strongly agreed or agreed to the impression of employing the flipped classroom method for teaching Radiology while 3.8% strongly disagreed or disagreed. O’Connor et al[8] demonstrated a 5.36% greater score in the flipped classroom method than in the didactic method. The flipped classroom group experienced higher task value (P<0.0001), less boredom (P<0.0001) and had greater enjoyment (P<0.0001).[8]
Durran-Guerora et al[17] demonstrated that the implementation of flipped classroom as a routine for teaching medical students had a significant impact on their grades and was perceived with high satisfaction rates which has the potential to propel the students to self-development. The difference in the grade of the students that were taught with the conventional lectures alone was significantly lower than those who received both.[17]
Radiology clerkship is the process where undergraduate medical students, at any level, rotate through every unit within the Radiology department and get to see how the plethora of radiological examinations are performed and the approaches at image interpretation.[2] In this study it was observed that 62% students had observed at least 5 ultrasound procedures, 93.7% students had not observed at least 5 CT scan procedures, 63.3% students had not observed the reporting of at least 10 films (radiographs) and 92.4% students had not observed any special procedure (barium swallow, barium meal or barium enema). In fact, 78.5% of the medical students in this study strongly disagreed or disagreed that they had sufficient patients to study during their posting. Bhogal et al[2] noted that the undergraduates who had a proper clerkship program were found to perform better in the assessment of radiological knowledge than those without one.
The size of the present exiting medical students in UNICAL is small which constitutes a limitation for this study. Furthermore, the use of structured closed ended questions limited the ability of the students to express themselves which would have been essential for the implementation of a far-reaching interventional measure.
CONCLUSION
Final year medical students in UNICAL have an appreciable knowledge of Radiology. This can be improved if the duration of Radiology education increases by early introduction into the pre-clinical class or other clinical courses, if the Radiology teaching methods are updated and if the quality of the learning environment is improved.
Recommendations
Integration of Radiology into course work of many Departments in the medical college of the clinical classes (surgery, internal medicine, pediatrics, obstetrics and gynecology, pathology etc) and pre-clinical classes (anatomy and physiology). This prevents the inevitable occurrence of information overload during the short span in which Radiology education is taught.
The flipped classroom method should be adopted for Radiology education
Radiologist should consistently attend courses that will improve Radiology education to undergraduate medical students.
Acknowledgments
Monumental gratitude to Professor Emmanuel Ekanem who inspired the concept of this research. We fervently thank the final year medical students for their willing participation in the study. The staff of the Radiology Department of University of Calabar Teaching Hospital were instrumental to an objective conduction of the questionnaire administration and we are sincerely grateful for their assistance.
Declaration of patient consent
The authors certify that they have obtained all appropriate patient consent.
Financial support and sponsorship
Nil.
Conflicts of interest
There are no conflicts of interest.
References
- Radiology for medical students (1925-2018): An overview. BJR Open. 2020;2:20190050.
- [CrossRef] [PubMed] [Google Scholar]
- Radiology in the undergraduate medical curriculum-who, how, what, when, and where? Clin Radiol. 2012;67:1146-52.
- [CrossRef] [PubMed] [Google Scholar]
- Medical student radiology education: Summary and recommendations from a national survey of medical school and radiology department leadership. J Am Coll Radiol. 2014;11:606-10.
- [CrossRef] [PubMed] [Google Scholar]
- A combination of traditional learning and e-learning can be more effective on radiological interpretation skills in medical students: A pre-and post-intervention study. BMC Med Educ. 2016;16:46.
- [CrossRef] [PubMed] [Google Scholar]
- An assessment of final-year medical students and interns awareness of radiation exposure to common diagnostic imaging procedures. Adv Radiol. 2014;2014:426909.
- [CrossRef] [Google Scholar]
- Knowledge, attitude and practice of radiology among physicians in a tertiary hospital in North-Central Nigeria. 2020. J Adv Med Med Res. 32:16-23. Available from: https://www.journaljammr.com/index.php/jammr/article/view/30395 [Last accessed on 2021 May 08]
- [CrossRef] [Google Scholar]
- An assessment of medical students' awareness of radiation exposures associated with diagnostic imaging investigations. Insights Imaging. 2010;1:86-92.
- [CrossRef] [PubMed] [Google Scholar]
- Flipping radiology education right side up. Acad Radiol. 2016;23:810-22.
- [CrossRef] [PubMed] [Google Scholar]
- Knowledge, attitude and practice of radiology among medical students at Sree Mookambika institute of medical sciences. Int J Res Rev. 2016;3:37-41.
- [Google Scholar]
- The utilisation of radiology for the teaching of anatomy in Canadian medical schools. Can Assoc Radiol J. 2012;63:160-4.
- [CrossRef] [PubMed] [Google Scholar]
- Medical student knowledge regarding radiology before and after a radiological anatomy module: Implications for vertical integration and self-directed learning. Insights Imaging. 2014;5:629-34.
- [CrossRef] [PubMed] [Google Scholar]
- An assessment of medical students' proficiency regarding the hazards of radiological examinations on the health of workers and patients: A cross-sectional study from Palestine. J Occup Med Toxicol. 2020;15:35.
- [CrossRef] [PubMed] [Google Scholar]
- Teaching Radiology to medical students-there is a need for change to better prepare students for clinical practice. Med Stud Educ. 2017;24:506-13.
- [CrossRef] [PubMed] [Google Scholar]
- Teaching medical students how to interpret chest X-rays: The design and development of an E-learning resource. Adv Med Educ Pract. 2021;12:123-32.
- [CrossRef] [PubMed] [Google Scholar]
- Undergraduate radiology teaching from the student's perspective. Insights Imaging. 2013;4:103-9.
- [CrossRef] [PubMed] [Google Scholar]
- Effectiveness of problem-solving exercises in radiology education for undergraduates. Natl Med J India. 2019;32:103-6.
- [Google Scholar]
- Blended learning: An effective methodology for teaching radiology to medical students. 2019. Rev Fac med. 67:273-7. Available from: http://www.scielo.org.co/scielo.php?script=sci_arttextandpid=S0120-00112019000200273andlng=en [Last accessed on 2021 May 08]
- [CrossRef] [Google Scholar]






